Pulse Oximeter Pleth (Plethysmograph)
Pulse oximeter can measure your SpO2 and blood flow fluctuation


Standard US shipping included (We ship internationally daily)
Product Description

A plethysmograph is an instrument for measuring changes in volume within an organ or whole body (usually resulting from fluctuations in the amount of blood or air it contains). A photoplethysmograph (PPG) is a plethysmograph that uses optical techniques. A pulse oximeter measures oxygen saturation level (SpO2) and is also a PPG. It can measure the change in the volume of arterial blood with each pulse beat. This change in blood volume can be detected in peripheral parts of the body such as the fingertip or ear lobe using a technique called photoplethysmography. The pulse oximeter that detects the signal is called a plethysmograph (or 'Pleth' for short).
Because of the nature of pulse oximeter, measuring the pressure from a pleth waveform has not been possible. However, the information has shown to be useful in diagnosis and in gauging the severity of illness in newborns. Many doctors use the pulse oximeter's pleth waveform as an early indication for cyclic changes in physiology. If the variability increases, it indicates a change in the intrathoracic/blood volume relationship.
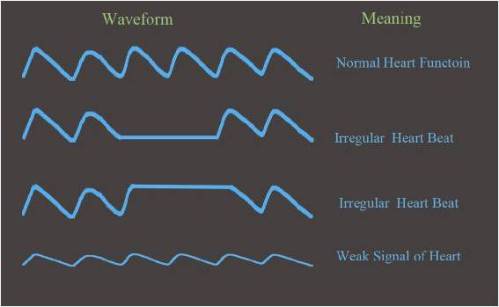
The blood flow is normally shown as a waveform using a bar or graph. It can provide useful information regarding the heart condition.
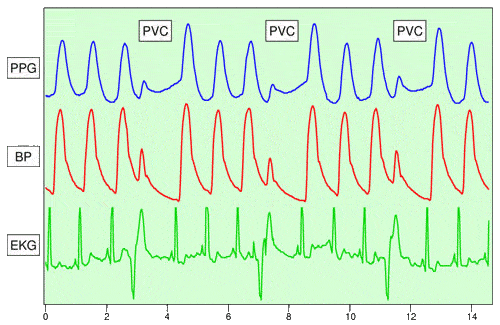
The following diagram illustrates the relationship among pleth (PPG), premature ventricular contraction (PVC), blood pressure (BP), and EKG.
Heart rhythm. Pleth is useful to detect irregular heart rhythm. The primary function of the heart is to supply blood and nutrients to the body. The regular beating, or contraction, of the heart moves the blood throughout the body. By watching the pleth waveform, the heart beating pattern is clearly displayed. When a heart patient is having discomfort, it is important to observe the pleth waveform and relate the information to his doctor. Since the discomfort is generally transient, a doctor may not be able to see the waveform during an office visit.
Signal strength. Weak signal is indicated by the amplitude of the waveform. If the signal is too low, it would affect the accuracy and functioning of the pulse oximeter. If your oximeter is not giving the correct result, check if the signal strength is too low.
There are several causes for the weak signal :
- Low blood perfusion
- Dirty sensors or LED lights
- Improper positioning of the oximeter
Low blood perfusion can be caused by cold temperature and the person's general health.
Respiration. During inspiration, intrapleural pressure decreases by up to 4 mm Hg which distends the right atrium, allowing for faster filling from the vena cava, increasing ventricular preload, and increasing the stroke volume. Conversely during expiration, the heart is compressed, decreasing cardiac efficiency and reducing stroke volume. However, the overall net effect of respiration is to act as pump for the cardiovascular system. When the frequency and depth of respiration increases, the venous return increase leading to increased cardiac output.
Respiration effects the cardiac cycle by varying the intrapleural pressure, the pressure between the thoracic wall and the lungs. Since the heart resides in the thoracic cavity between the lungs, the partial pressure created by inhaling and exhaling affects the pressure on the heart and hence the blood flow volume.
Only more advanced pulse oximeter would provide the waveform. Read this article "Photoplethysmograph" for more information how the waveform is related to breathing, hypovolemia, and other circulatory conditions.
Finger pulse oximeters MD300C23, MD300C21 and CMS50EW all have this feature.

A plethysmograph is an instrument for measuring changes in volume within an organ or whole body (usually resulting from fluctuations in the amount of blood or air it contains). A photoplethysmograph (PPG) is a plethysmograph that uses optical techniques. A pulse oximeter measures oxygen saturation level (SpO2) and is also a PPG. It can measure the change in the volume of arterial blood with each pulse beat. This change in blood volume can be detected in peripheral parts of the body such as the fingertip or ear lobe using a technique called photoplethysmography. The pulse oximeter that detects the signal is called a plethysmograph (or 'Pleth' for short).
Because of the nature of pulse oximeter, measuring the pressure from a pleth waveform has not been possible. However, the information has shown to be useful in diagnosis and in gauging the severity of illness in newborns. Many doctors use the pulse oximeter's pleth waveform as an early indication for cyclic changes in physiology. If the variability increases, it indicates a change in the intrathoracic/blood volume relationship.
The blood flow is normally shown as a waveform using a bar or graph. It can provide useful information regarding the heart condition.

The following diagram illustrates the relationship among pleth (PPG), premature ventricular contraction (PVC), blood pressure (BP), and EKG.

Heart rhythm. Pleth is useful to detect irregular heart rhythm. The primary function of the heart is to supply blood and nutrients to the body. The regular beating, or contraction, of the heart moves the blood throughout the body. By watching the pleth waveform, the heart beating pattern is clearly displayed. When a heart patient is having discomfort, it is important to observe the pleth waveform and relate the information to his doctor. Since the discomfort is generally transient, a doctor may not be able to see the waveform during an office visit.
Signal strength. Weak signal is indicated by the amplitude of the waveform. If the signal is too low, it would affect the accuracy and functioning of the pulse oximeter. If your oximeter is not giving the correct result, check if the signal strength is too low.
There are several causes for the weak signal :
- Low blood perfusion
- Dirty sensors or LED lights
- Improper positioning of the oximeter
Low blood perfusion can be caused by cold temperature and the person's general health.
Respiration. During inspiration, intrapleural pressure decreases by up to 4 mm Hg which distends the right atrium, allowing for faster filling from the vena cava, increasing ventricular preload, and increasing the stroke volume. Conversely during expiration, the heart is compressed, decreasing cardiac efficiency and reducing stroke volume. However, the overall net effect of respiration is to act as pump for the cardiovascular system. When the frequency and depth of respiration increases, the venous return increase leading to increased cardiac output.
Respiration effects the cardiac cycle by varying the intrapleural pressure, the pressure between the thoracic wall and the lungs. Since the heart resides in the thoracic cavity between the lungs, the partial pressure created by inhaling and exhaling affects the pressure on the heart and hence the blood flow volume.
Only more advanced pulse oximeter would provide the waveform. Read this article "Photoplethysmograph" for more information how the waveform is related to breathing, hypovolemia, and other circulatory conditions.
Finger pulse oximeters MD300C23, MD300C21 and CMS50EW all have this feature.
Shipping Information
Shipping Weight: 0.00 Pounds
Availability: In stock! Ready to ship.
Shipping Cost: US Shipping included! Int'l Shipping calculated at checkout
In-stock items are normally shipped within 24-48 hours on business days. For special handling or overnight shipping, please call us at 281-664-1209.
Manufacturer Information
Manufacturer:
Item Code:
Product belongs to these categories...
Pulse Oximeters
Resource: Healthcare

